Insulin at 100: Challenges Faced By Kenyans With Type 1 Diabetes
2021 marks the centenary of the discovery of therapeutic insulin in 1921. At the same time, a new study by Médecins Sans Frontières (MSF) shows insulin can be stored at up to 37°C after opening and remains viable for several weeks. The findings also reveal the difficulties Kenyans dependent on insulin face.
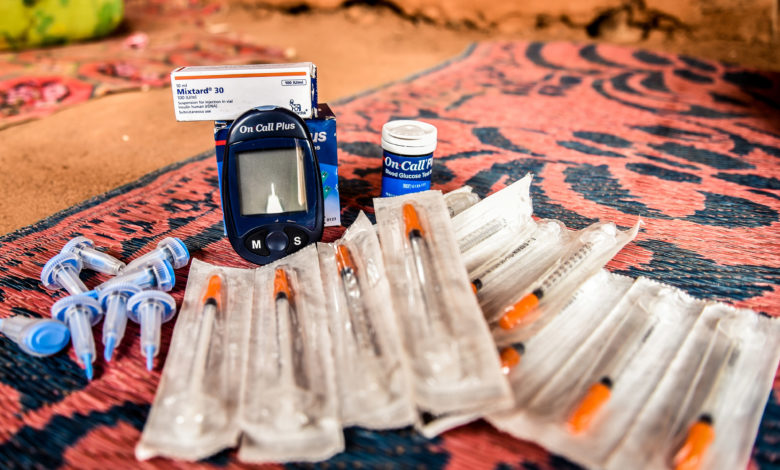
A new study reveals that insulin can be kept at higher temperatures during the period of use. The study also opened the lid on the difficulties faced by thousands of Kenyans with Type 1 Diabetes.
These are people who require daily injections with insulin to survive. As the world marks 100 years since the discovery of therapeutic insulin in 1921 in Toronto, Canada ,this study brings their plights to the fore.
According to the World Health Organization guidelines, insulin vials must be stored at between 2° and 8°C until opened, after which they can be stored at 25°C for four weeks.
This means patients need to have electricity and a home refrigerator. Otherwise they have to take tedious daily trips to chemists or health facilities for injections.
Relief for patients
But a joint study by Médecins Sans Frontières /Doctors Without Borders (MSF) and University of Geneva (UNIGE) published on February 3,2021, in Plos One, shows that the world was wrong about this all along.
Plos One is a peer-reviewed open access scientific journal published by the Public Library of Science. The journal covers primary research from any discipline within science and medicine.
The study, carried out in Dagahaley refugee camp in Garissa County, Kenya demonstrates that a range of insulins can be stored at temperatures ranging from 25 to 37°C for a four–week period of use.
This range of temperature is also the usual temperature in most parts of Africa.
“These results can serve as a basis for changing diabetes management practices in low-resource settings, since patients won’t have to go to hospital every day for their insulin injections,” said Dr Philippa Boulle, MSF Non-Communicable Diseases Advisor.

The results, of the study also reveal the difficult investments Kenyans living with Type 1 Diabetes must make just to stay alive.
Type 1 diabetes is a chronic condition in which the pancreas produces little or no insulin, a hormone that helps glucose pass from the blood into body cells for energy.
Complications caused by diabetes
Insulin deficiency leaves too much glucose in the blood. According to Mayo Clinic, this can cause heart and blood vessel disease, nerve damage, kidney damage. It can also lead to eye damage, foot damage, skin and mouth conditions, and even pregnancy complications.
In Type 2 diabetes, the body actually produces insulin but is unable to use it effectively.
The 2015 STEPwise Survey for Non-Communicable Diseases (NCDs) placed the prevalence of diabetes in Kenya at 3.3 per cent of the entire population.
The Kenya STEPs survey is a nationally representative survey to collect comprehensive information on risk factors for NCDs and injuries.
The International Diabetes Federation says the number of Kenyans with diabetes has grown from 460,000 in 2017 to 700,000 at the end of November 2019. About five to 10 per cent have Type 1 diabetes.
While Type 2 can be managed with lifestyle changes, Type1 requires daily injections of insulin, sometimes three times daily, to help sugar enter the body’s cells.
Dr Boulle of MSF said this is where the challenges experienced by patients begin.
“For far too long, we were unable to send people with diabetes back to their homes with insulin, due to its cold-storage requirements. Some of these people travel long distances daily, while others relocate near the clinics to access insulin injections,” she said in a statement published by MSF.
Poverty a challenge to treatment
Refrigerators and electricity are largely unaffordable by Kenyans in the poor northern region. Poverty levels are above 60 per cent, according to the 2015/2016 Kenya Integrated Household Budget Survey.
For instance, in Garissa County, where the MSF study was carried out, 65.5 per cent of residents are considered poor.
Once a vial has been opened, insulin can be stored at ambient temperature during the usual four to six weeks period of use, depending on the brand and type of insulin.
According to manufacturers’ specifications, the study says, the maximum ambient temperature should not exceed 30°C during this period.
The MSF team said they found that the temperatures in homes in the Dagahaley refugee camp fluctuate between 25°C at night and 37°C during the day.
“The risk is that insulin, a protein, precipitates under the influence of heat. In other words, it would begin to form ‘flakes’. Since the insulin is no longer in solution, it can’t be injected,” explains Leonardo Scapozza, a professor of the School of Pharmaceutical Sciences in University of Geneva’s Faculty of Sciences.
The study says physical degradation is irreversible and leads to fibril formation.
It also confirmed for the first time that insulin vials can be used for up to four weeks even in hot weather without being refrigerated.
“The common practice of systematically discarding any insulin vial that has been exposed to heat may be re-evaluated,” the authors said.
Call for endorsement

As the world marks 100 years of discovery of therapeutic insulin, MSF is now calling on the WHO to endorse these findings and asks pharmaceutical corporations to amend their guidelines.
Insulin storage is not the only challenge patients in low-resource settings face. Testing for diabetes, access to insulin itself and proper diets are the other life-threatening challenges.
According to the Christian Health Association of Kenya (Chak), which runs all mission hospitals in Kenya, many diabetics patients do not even know their status.
“The majority of Kenyans (87.8 per cent) have never done a blood sugar test in their lifetime. Yet nearly two per cent of Kenyans (nearly one million people) have raised blood sugar levels according to the Kenya STEPwise Survey for NCDs,” Chak says in a 2020 report.
Access to insulin is another major challenge. Costs have remained high for the last 100 years.
In October 2019, the International Journal of Health Planning and Management published a study on costs incurred by diabetes patients in Kenya.
“The most expensive antidiabetic regimen was metformin and insulin mean annual cost Sh 15,636,” the authors say.
Extra costs
The administration of insulin comes along with other costs such as insulin pumps, insulin pens, pen tips and tests.
“Overall, the mean annual direct patient cost was Sh 53,907. Medicines accounted for 52.4 per cent, transport 22.6 per cent, user charges 17.5 per cent, and food 7.5 per cent of total direct costs,” the authors say.
Although the National Hospital Insurance Fund offsets many of these charges, beneficiaries need to pay the Sh 500 insurance premiums and sometimes the products are not available in public health facilities.
“High incidence of catastrophic costs suggests diabetes services are unaffordable to the majority of diabetic patients and illustrate the urgent need to improve financial risk protection to ensure access to care,” the study says.
What journalists should do:
- Find out if the Ministry of Health keeps a proper register of Kenyans with diabetes. Use the register for factual reporting where data is needed.
- Talk to people who are living with diabetes or taking care of diabetic patients to share their experiences on the costs incurred.
- Find out what costs are covered by the National Health Insurance Fund (NHIF) and which ones are covered directly by patients. Also find out if private insurance companies cover diabetes and to what extent.
- Check with health institutions and the Kenya Medical Supplies Authority (KEMSA) to find out the availability of insulin in all parts of Kenya.
- Investigate challenges faced by patients in their daily lives at home, work and school.
- Research how other countries manage diabetes.
Pretty nice post. I just stumbled upon your weblog and wished to mention that I have truly loved browsing your blog posts. In any case I will be subscribing in your rss feed and I am hoping you write again soon!
I do agree with all of the ideas you have presented in your post. They are very convincing and will definitely work. Still, the posts are too short for newbies. Could you please extend them a bit from next time? Thanks for the post.